Our success stories
Read the stories from the teams behind some of our key achievements, including bringing drugs to market, licensing, forming startups and developing...
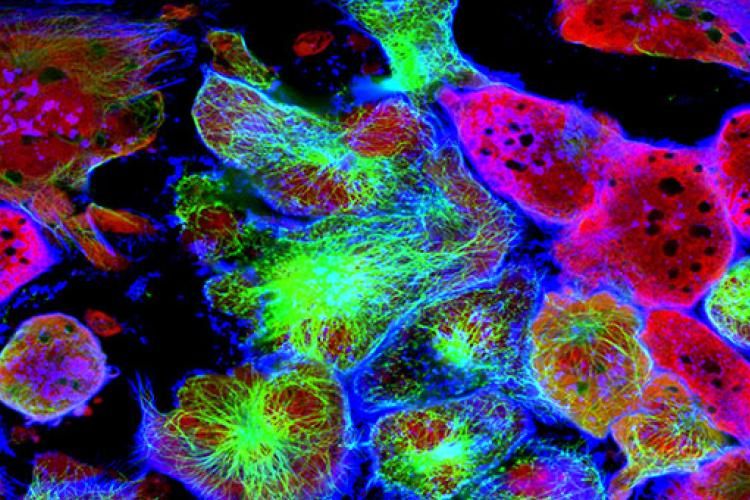
The reagents you need to get the most from your science are vital. This is why CancerTools.org have established a community approach to accessing – and depositing – tools to help accelerate cancer research. Here we learn how cancer patient-derived organoids from Japan’s Fukushima Medical University became the latest technology to be made available…
A little over a decade ago, cancer biologists Hirosumi Tamura and Gen Hiyama at Fukushima Medical University, set out to make some cell lines from patients’ tumours. Patient-derived cell lines have been a staple of cancer research for decades – a single cell type, usually the most prolifically dividing one, is isolated from a person’s cancer and maintained indefinitely in culture.
But there are well known limitations. A cell line does not capture the complexity of a cancer as it develops inside a person. And sometimes the differences between such models and the clinical reality they are intended to mimic can be simply too great – with, for example, drugs that potently stunt the growth of a cell line doing little to halt the progression of patients’ disease.
As it was, in Fukushima in 2012, Tamura and his team were struggling to make cell lines. They had begun using standard techniques – taking chunks of tumours, they separated out the constituent cells using enzymes that digested away the extracellular proteins that bound them together, then plated the cells on culture dishes. But too often non-cancerous cells from the sample – such as fibroblasts that naturally continue to divide – swamped the dishes.
Eventually, the team tried something new. Chopping tumour samples into roughly 1-millimetre-cubes, they attempted to grow these undigested chunks in suspension.
Floating in culture medium, the tumour samples survived. And, remarkably, the majority of non-malignant bodily cells gradually fell away. Left behind was a cancer organoid – a 3D mass composed primarily of a heterogenous mix of cancer cells.
When Tamura’s lab performed histology on the organoids side-by-side with histology on samples of the tumours from which each had been derived, they saw striking similarities in the way the cancer cells were organised.
Then, focusing on an endometrial cancer, they ran large scale gene expression analyses of the organoids and their parent tumours. Again, the parallels between them were pronounced. What’s more, genetically speaking, the organoids looked more like the original cancers than they did cell-line models of endometrial cancer.
“Compared with cell lines,” Tamura says, “the biggest difference is that the organoid better resembles the characteristics of the clinical tissue.”
On top of this, organoids retain a fundamental advantage of cell lines: because the organoids can be grown and expanded in culture, then divided to give abundant identical samples, it is still possible to run high throughput screens using them.
When Tamura and Hiyama’s group published the first description of their organoids in 2018, they reported how they had adapted them to test the efficacy of anticancer drugs using 96- or 384-well microplates. And, again, the organoids and cell lines diverged in their sensitivity to a range of anti-cancer drugs, with the organoids better reflecting the effectiveness of various drugs in a clinical setting.
Follow up papers published in 2019 and 2021, showed how the group has extended the types of drugs they can screen on organoids, including small-molecule inhibitors, monoclonal antibodies, and antibody-drug conjugates. They also demonstrated how organoids can be combined with immune cells to assess the transformative set of treatments that are immunotherapies.
Besides cell lines, the other dominant model system used for drug screening – and many other types of experiments – is xenografts, where human cancer samples are implanted in immunocompromised mice to develop into tumours. But while this system recapitulates the clinical scenario better than cell lines, it is expensive and time-consuming, making it unsuitable for high-throughput screening.
Tamura thinks that organoids offer a sweet spot between the two older model types. “The development of effective anti-cancer drug has been extremely difficult due to cancer’s numerous complexities,” he says. “The main advantage of these organoids – their resemblance to clinical tissue – should make a key contribution to solving this issue.”
The development of effective anti-cancer drug has been extremely difficult due to cancer’s numerous complexities. The main advantage of these organoids – their resemblance to clinical tissue – should make a key contribution to solving this issue.
For this reason, Tamura, Hiyama and colleagues wanted to make their organoids available to as many researchers as possible.
With the lab having developed over 100 organoids from sixteen different cancer types – all of them cryopreservable – Tamura and Hiyama first partnered with Summit Pharmaceuticals International, the technology transfer partner of Fukushima Medical University. But then, early last year, a seemingly perfect opportunity presented itself.
The researchers and the team at Summit read about CancerTools.org – the branch of CRUK that identifies useful cancer research reagents and makes them as widely and easily available to the research community as possible.
“We thought,” Tamura says, “this would be the best opportunity to introduce Fukushima patient-derived organoids to the global market.”
The lab and Summit were learning about CancerTools.org because the operation was promoting its relaunch.
“The business is not new, the brand is new,” says Pawanbir Singh, CancerTools.org’s Head of Marketing. CRUK has had a small, largely autonomous franchise for distributing research tools for around 40 years now. It is a profitable operation, Singh explains, but “all the profits go back either to the researchers directly or to funding programs that the charity manages.”
Last year’s relaunch and renaming as CancerTools.org reflect a change in strategy, says Singh. Previously, the unit had mainly identified reagents developed by cancer researchers and acted as a conduit for placing them with businesses that would then sell them to the community. Now, though Singh, says, “we are trying to become a more of a direct to end user brand.”
Currently, if a scientist reads a publication and learns of a new reagent that they think would help their research, they must write to the researchers who developed it, ask politely if they can have it, then, typically enter into long, drawn out process of material transfer arrangements and other logistics before they can access them, says Singh. At CancerTools.org, he says, “we take all that pain from these researchers.”
The first thing CancerTools.org must do to serve as this intermediary is to identify suitable new tools. Singh says there are two ways in which this happens. First, tools come from scientists who have received CRUK funding. Second, he says, they have fostered relationships with around 180 research outfits worldwide, through which academics are encouraged to contribute any new tools or technologies they make – this is precisely what Tamura and his colleagues did.
Any such reagents remain the intellectual property of their developers, Singh says, with CancerTools.org typically working with Technology Transfer Offices to license the product in a mutually beneficial manner.
While there are several companies that serve a similar function, acquiring and selling useful reagents, Singh says that these tend to specialise solely in one type of reagent – say, antibodies or cell lines – and are not especially interested in the research objectives of their customers. CancerTools.org is different because it collates many types of research tools and is centred on the shared research goal of its target audience. “We have antibodies; cell lines; we have organoids; we have viral vectors; proteins; small molecules,” says Singh. “We are working across the spectrum, but our focus is supporting cancer research.”
Indeed, the outfit currently has a portfolio of around 4,000 products – which also includes lines of genetically modified mice plus specialist culture media for maintaining primary cells and cell lines. “And the portfolio is ever increasing,” Singh says, with the team always open to branching out into new state of the art technologies if that technology can drive cancer research forward.
Often these products are not themselves going to be hugely profitable – in the way that a cancer drug or diagnostic tool might be – meaning that their developers may not rush to commercialise them. But they are nevertheless potentially very valuable to researchers seeking to ultimately develop those transformative products and so streamlining commercialisation and distribution of these reagents is crucial and a role that CancerTools.org fulfils.
Once suitable products have been identified and licensed, they are brought to CancerTool.org’s production facilities in Cambridge. There, an outsourced team of experts in cell culture, biochemistry, bioengineering and any other necessary skill set, stores, processes and produces the relevant reagents. This inhouse expertise also means they can offer extensive technical support to anyone using its products.
“We want researchers to come to us to deposit their reagents”, Singh says, “because we are the first of its kind; a non-profit biorepository of research materials with global coverage.”
We want researchers to come to us to deposit their reagents because we are the first of its kind; a non-profit biorepository of research materials with global coverage.
Having recently attended multiple conferences where the buzz around organoid biology is palpable, Singh speaks enthusiastically about making these reagents easily available to the cancer research community.
At present, CancerTools.org is storing and preparing to produce 46 of the organoid lines from Tamura and Hiyama’s group– with more than 50 other lines available in Japan – and talking to several potential first users.
Any research group that purchases one of these organoid lines will get a product that they can maintain and expand to use indefinitely in their own labs. In addition to detailed technical protocols, purchasers can access the relevant characterisation data, that includes information about the different cell types present in each type of organoid and data regarding these cells’ genomes, morphology and gene expression profiles.
“There are multiple applications – you can replicate anything that you would do with a cell line,” Singh says of these organoids, highlighting how large scale drug screens can easily be run on them, aspects of disease progression can be modelled and also immunotherapies tested on them. “And because these are not cell lines, they’re organoids,” he says, “the results are more relevant, because these organoids are more representative of clinical tissues.”
Because of these advantages and because organoid biology is moving so quickly – both in cancer research and biomedical investigation more broadly – Singh says that CancerTools.org want to be central to this field. They are, for instance, continuing to work with the research team at Fukushima to optimise processes and ancillary reagents required for growing organoids for different applications. Plus, they are encouraging other academic labs to deposit further organoid lines with them.
With Tamura and Hiyama convinced of the value and potential of the organoids their lab has created – and having seen their team develop robust methods for maintaining and utilising this resource – he is thrilled to be working with CancerTools.org. “Fukushima Medical University and Summit Pharmaceuticals International,” they say, “hope to see the use of their patient-derived organoids by as many global researchers in this field as possible.”
Explore the reagents and tools available through CancerTools.org
Find out how to contribute
Hirosumi Tamura
Hirosumi Tamura is Assistant Professor Fukushima Medical University.
Gen Hiyama
Gen Hiyama is Associate Professor at Fukushima Medical University.
Pawanbir Singh
Pawanbir Singh is head of marketing for CancerTools.org.
This story was first published on Cancer News on cruk.org


